Bowel & Bladder
Overview
This chapter will review how bladder and bowel changes can affect your sexual life and relationships. It will also explore strategies to limit accidents, to talk more comfortably about this with a partner and maintain feelings of sexiness.
MYTH
If I have a Foley catheter in place I can’t have sex.
FACT
Yes you can!
Introduction
Your bowel and bladder’s main function is to remove waste from your body. There are many physiological processes that take place from the time fluid and food enters your body, to the time it is eliminated (don’t worry, we won’t go into the specifics in this chapter).
The nerves involved with bowel and bladder function are closely connected to the nerves involved with sexual function. Oftentimes, if there are changes to bowel and bladder function there will also be changes to sexual functioning and vice versa.
What’s Different Now?
Following spinal cord injury there is a change in the communication system between the nerves, the spinal cord, and the brain. For some people this can cause changes to bowel and bladder function.
Common changes to bladder function:
- If your injury is below T12 this means you likely have a flaccid bladder – unable to empty your bladder on command. Your bladder tends to fill up without you feeling this fullness. If it gets too full your bladder may leak and you run the risk of damaging your bladder by over filling it and the fluid backing up into your kidneys. Typically, intermittent catheterizations are used to manage this type of bladder.
- If your injury is above T12 you likely have a spastic bladder meaning your bladder will empty itself without your control when it is full. Again, you may not sense the bladder fullness. You may leak small or large amounts of urine. Typically, this is managed with medications and intermittent catheters. You may also require the use of condom catheters or incontinence briefs.
- If you have an incomplete SCI, you may have some sensation of bladder fullness, you may also be able to pass urine without assistance. However, catheters may need to be used because you are unable to empty your bladder completely.
- In some cases, a Foley catheter is used to manage bladder function. This strategy can be used for any level of injury.
Common changes to bowel function:
- If your level of injury is below T12 you likely have a flaccid bowel meaning you are unable to empty your bowel on command. The bowel tends to fill up without you feeling this fullness. If it gets too full you may experience bowel leakage of varying consistencies (i.e. mucous, hard stool (poo), or liquid stool). Typically this is managed with a daily or a twice a day bowel regime which includes oral medications (pills) and requires the manual removal of stool.
- If your injury is above T12 you likely have a spastic bowel meaning your bowel will empty itself when it fills up. Again, you may not sense the bowel fullness. You may pass small or large amounts of stool by accident. Typically, this is managed with an every other day bowel regime which includes pills, medicated or glycerine suppositories and/or digital stimulation (dig stim) to trigger emptying.
- If you have an incomplete SCI, you may have some sensation of bowel fullness, you may also be able to pass stool without assistance. However, some of the strategies mentioned above may need to be used.
These changes can have an impact on sexual self-esteem and confidence. People often worry about:
- having accidents in social settings and during sex
- how to discuss bowel and bladder issues with partners
- how to be sexual with a Foley catheter
- feeling or smelling unclean
What Can I Do About It?
Learn about the specific types of bowel and bladder changes that are common with your level of SCI – do you have a flaccid or spastic bowel/bladder? Learn about the medications, tools, aids, and/or devices that can assist you with your bowel and bladder routine (e.g. stool softeners, laxatives, suppositories, digital stimulation tools, bladder medications, catheters, condoms, etc). For more information, talk to your physiatrist, urologist, doctor, or nurse continence advisor.
Things are going to be different now; however, being familiar with how your bowel and bladder are working and establishing a routine will help your confidence and willingness to engage in social and sexual activities.
What Do I Need to Know?
I’m worried about having a bowel or bladder accident during sex.
- Have a reliable and predictable bladder and bowel program in place
- Use a catheter to urinate prior to engaging in sexual activity (BE MINDFUL: after laying down, fluid shift in your body may cause your bladder to fill up again)
- Plan sexual activities on your bowel days as there is more of a chance your bowels will be empty
- Talk to your partner about the potential for accidents
- Try to avoid sexual positions that put extra pressure on your bladder or bowel
- Keep extra supplies, towels and pads close at hand
I pee with orgasm, is this normal?
Pelvic floor physiotherapy can be helpful only if you have some sensation and ability to contract the pelvic floor muscles.
How can I talk to my partner about a bowel or bladder accident during sex?
Having said that, life is unpredictable and accidents do happen. Talking to your partner ahead of time can help you prepare in case something does happen. Don’t forget that sex can be messy for the average couple too. It isn’t unusual to need to “clean up” after sex, and there are even products available for the bedroom to help you do just that – one example is the Liberator Throe – a nice romantic blanket that can cover your bed, is moisture-proof and can be laundered.
How can I have sex with a Foley catheter?

Foley Catheter Plug
Women:
The foley catheter can be left in place (this is because the urethra is above the vagina). It is important to be mindful of any potential tugging or pulling on the catheter. Taping the catheter to your thigh or abdomen to anchor the catheter and keep it in place is recommended. Your leg bag or drainage bag can either be left attached or can be removed and plugged with a catheter plug. Important note: plugging a catheter can cause AD if your bladder capacity has shrunk due to long-term foley placement.
Men:
Your foley catheter can be left in place for sexual activity. Here’s how: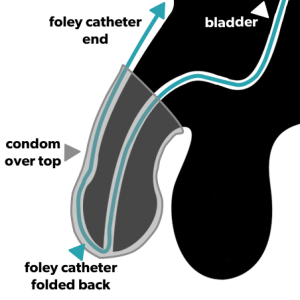
- Leave some slack at the tip of the penis
- Fold the catheter over the length of the penis
- Put a condom over the penis to secure it in place
- Tape the catheter to your abdomen or thigh to anchor it in place
- The leg bag or drainage bag can either be left attached or can be removed and plugged with a catheter plug. Important note: plugging a catheter can cause AD if your bladder capacity has shrunk due to long-term foley placement.
Some men and women prefer to remove their foley catheter for intercourse. If you decide to do this, you or your partner need to know how to re-insert a new, sterile foley catheter OR have a trained care giver or nurse re-insert it for you.
How can I feel sexy when I have to wear an incontinence brief because of bowel and bladder accidents?
- Changing briefs and pads regularly can help you to feel fresher during the day
- Carry moist towelettes with you for on-the-go cleansing
- There are many different types of briefs and underwear pads on the market, choose one that is comfortable for you
- Discuss with your health care provider how you can minimize accidents if they are occurring on a regular basis
RESOURCE
Bowel Management Info Poster
My Role
Establish a bowel and bladder regime that works for your type of injury. A reliable and predictable routine is going to boost your confidence in social and sexual settings. Become aware of the resources available to you if you are having difficulties in this area.
Who Can Help Me?
Your urologist and nurse continence advisor or urology nurse are the best choice to address what might be causing bladder accidents and provide ways to deal with them. Your Physiatrist (Rehab Doctor) can help you strategize ways to address the bladder and bowel problems you’re experiencing, and your family physician (GP) can prescribe medications that may assist in minimizing accidents.
Peers can also be a helpful resource to give you ideas and suggestions about maintaining your bowel and bladder. Try your local rehabilitation hospital or spinal cord injury organization to get involved in a peer group or speak with a peer mentor.
RESOURCE
Do You Know Your Bladder?
Conclusion
Despite the changes to your bowel and bladder function, you are still a sexual person. Being involved in your bowel and bladder care can provide you with the skills and confidence necessary to deal with bowel or bladder accidents when they happen. Communication about these concerns to a partner, having supplies with you while you’re out, and knowing your resources will help you feel more comfortable in your relationship (if in one), dating, or social life.
Bowel & Bladder Resources
Websites
Bladder Management - General bladder management principles after SCI, Christopher and Dana Reeve Foundation.
Bladder Management - Module within Spinal Cord Injury BC x G.F. Strong's Living with SCI resource website.
Bowel Management - Module within Spinal Cord Injury BC x G.F. Strong's Living with SCI resource website.
Guides & Downloadable PDF's
Bladder Management following Spinal Cord Injury: What you should know (PDF) - Consortium for Spinal Cord Medicine.
Bladder Management (PDF) - G.F. Strong Rehabilitation Centre; to print, choose landscape, 8.5 x 11"
Bowel Management (PDF) - G.F. Strong Rehabilitation Centre; to print, choose landscape, 8.5 x 11"
Videos
Managing Bodily Functions - Sexuality After SCI
SCI-U: Bladder course - A free, peer-based online course.
SCI-U: Bowel course - A free, peer-based online course.
Check out this chapter's Video Playlist.
VIDEO
Check out the video playlist for this chapter!


